MRCP Part 2 Written Exam Format
- The MRCP Part 2 Written Exam has 200 questions in a two-paper format held over one day.
- Each paper in the Part 2 Written Examination is 3 hours in duration and contains 100 multiple choice questions.
| Specialty | Number of questions |
|---|---|
| Cardiology | 19 |
| Dermatology | 9 |
| Endocrinology and metabolic medicine | 19 |
| Gastroenterology | 19 |
| Geriatric medicine | 9 |
| Haematology | 9 |
| Infectious diseases and GUM | 19 |
| Neurology | 17 |
| Nephrology | 19 |
| Oncology and palliative medicine | 9 |
| Ophthalmology | 3 |
| Psychiatry | 3 |
| Respiratory medicine | 19 |
| Rheumatology | 9 |
| Therapeutics and toxicology | 18 |
| 200 |
- NB: This should be taken as an indication of the likely number of questions – the actual number may vary by up to 2%.
A proportion of the questions will be on adolescent medicine.
MRCP Part 2 Written Exam content
- The questions will usually have a clinical scenario, may include the results of investigations and may be illustrated with images such as:
- clinical photographs,
- pathology slides,
- inheritance trees,
- ECGs, X-rays,
- CT and MR scans,
- echocardiograms.
- Questions are asked about the diagnosis, investigation, management, and prognosis of patients using multiple choice questions in ‘best of five‘ format.
- This format, in addition to testing core knowledge and comprehension, also assesses the ability to interpret information and to solve clinical problems.
- There will be five options: one correct answer and four alternatives to the correct answer.
- The four distractors will be closely related to the preferred option but less correct, therefore acting as plausible alternatives.
- The candidate chooses the best answer from the five possible answers. Each correct answer is awarded one mark; there is no negative marking.
- The results of each examination are benchmarked using a process of test equating which ensures that the pass mark is adjusted for the difficulty of the paper and the ability range of the candidates.
- The reliability of every examination is monitored, and provides assurance that the results identify those candidates who have achieved the required standard.
- A detailed explanation of the marking system used for the MRCP(UK) Part 2 Written Examination can be viewed on the exam pass mark page of our website and in the MRCP(UK) Regulations.
Sample MRCP Part 2 Written Exam questions
1. A 67-year-old woman was referred with a 3-month history of painful legs, malaise and weight loss. She had had type 2 diabetes mellitus and hypertension for 18 years. Her medication was gliclazide 160 mg twice daily, ramipril 2.5 mg daily and atorvastatin 20 mg daily. On examination, her BP was 145/90 mmHg. She had some tenderness over her spine and legs. Investigations:
| serum sodium | 138 mmol/L (137–144) |
| serum potassium | 5.5 mmol/L (3.5–4.9) |
| serum creatinine | 240 µmol/L (60–110) |
| serum corrected calcium | 1.80 mmol/L (2.20–2.60) |
| eGFR (MDRD) | 19 mL/min/1.73 m2 (>60) |
| serum phosphate | 1.60 mmol/L (0.80–1.45) |
| plasma parathyroid hormone | 22.2 pmol/L (0.9–5.4) |
What therapy is most likely to correct the calcium and parathyroid hormone concentrations?
2. A 52-year-old man presented with a 4-month history of altered bowel habit with occasional bright-red blood per rectum. Colonoscopy showed an annular sigmoid tumour, and histology confirmed an adenocarcinoma. A staging CT scan showed two adjacent 1-cm lesions in the right lobe of the liver, highly suspicious for liver metastases. What is the most appropriate management?
3. A 53-year-old man presented with a 2-week history of diarrhoea associated with cramping abdominal pain. He was passing up to 15 very loose and watery stools per day. He had no blood in his stools. He had undergone a heart transplant 2 years previously, and his medication comprised ciclosporin, prednisolone, aspirin and ramipril. Investigations:
| haemoglobin | 110 g/L (130–180) |
| white cell count | 12.5 × 109/L (4.0–11.0) |
| serum urea | 14.4 mmol/L (2.5–7.0) |
| serum creatinine | 135 µmol/L (60–110) |
| serum CRP | 35 mg/L (<10) |
| stool culture | negative |
| stool microscopy | cysts identified on modified acid-fast stain |
What is the most likely pathogen?
| Arterial blood gases breathing air | |
| PO2 | 6.8 kPa (11.3–12.6) |
| PCO2 | 9.8 kPa (4.7–6.0) |
| pH | 7.25 (7.35–7.45) |
| H+ | 56 nmol/L (35–45) |
| bicarbonate | 32 mmol/L (21–29) |
| base excess | +10.0 mmol/L (±2.0) |
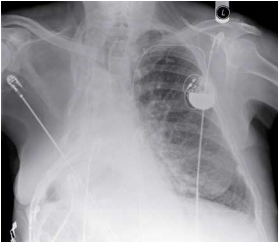
What is the most appropriate treatment?
5. A 75-year-old man presented with widespread aches and pains. He had a 20-year history of haemodialysis for end-stage renal disease. An X-ray of his hand was performed (see image).
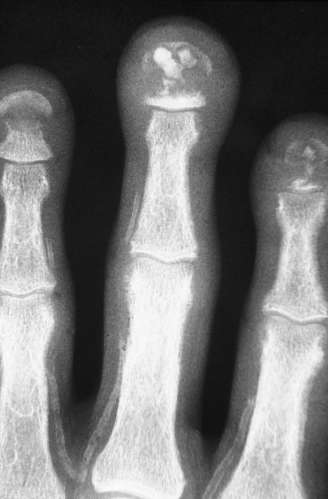
What is the most likely diagnosis?
Also read:
- MRCP part 2 FAQs
- MRCP part 2 News
- MRCP part 1 MCQs in youtube channel “Knowledge Pro”
- MRCP part 1 MCQs in youtube channel “Fast Track”
- All You Need to Know About the MRCP Part 1
- MRCP Part 1 Exam format
- All You Need to Know About the MRCP Part 2
- MRCP Part 2–MRCP PACES
- Preparation for MRCP PACES
- MRCP PACES examination format